Editorially Independent Content
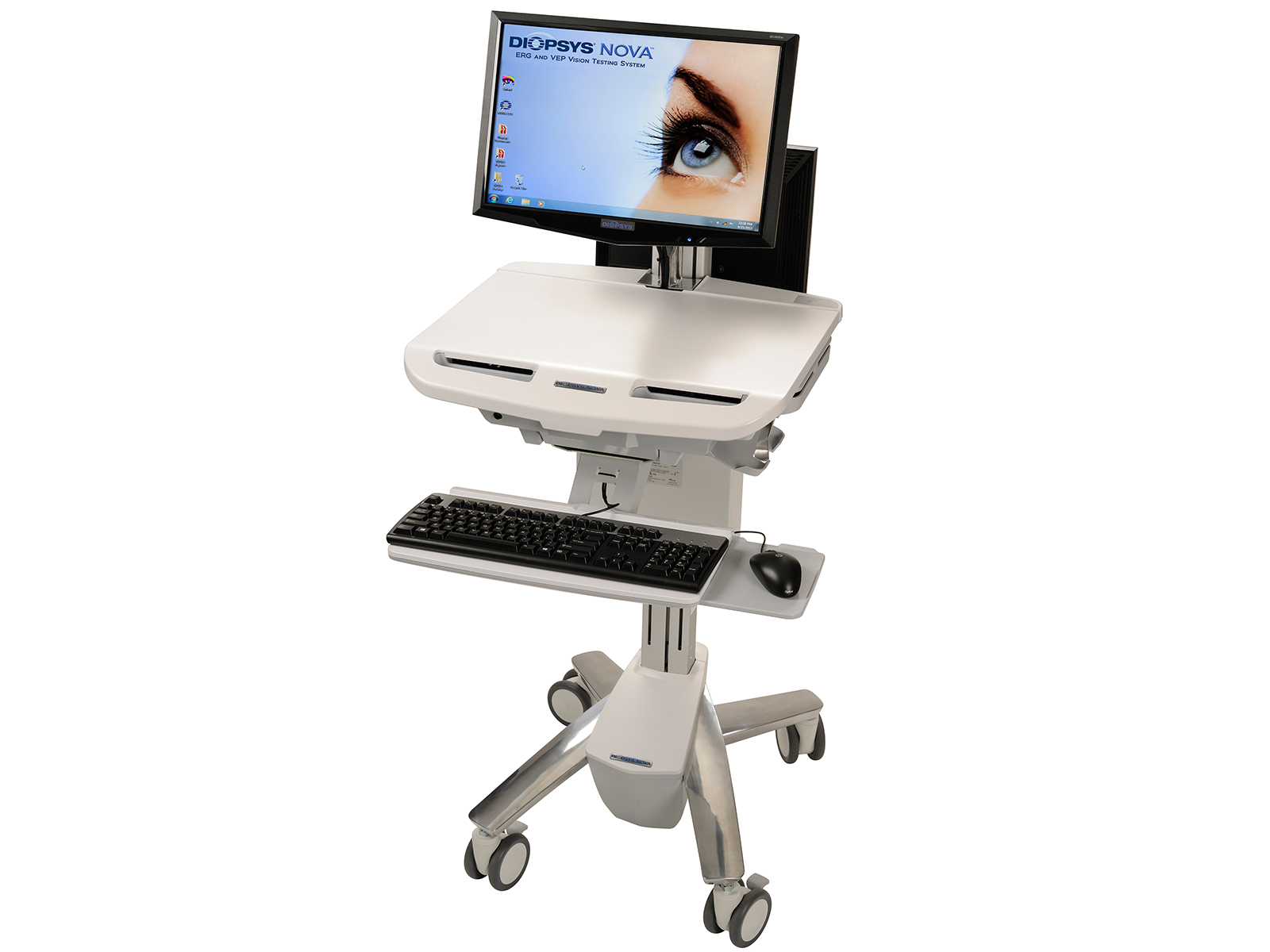
The Diopsys Visual Evoked Potential (VEP) and the Diopsys Pattern Electroretinography (ERG), which are modules of the Diopsys’ NOVA suite of vision tests, help me make clinical decisions and diagnose visual disorders and disease sooner. For patients with early glaucoma, ocular hypertension, drug toxicity such as Plaquenil, or other conditions, the pattern ERG and VEP modules can detect a disorder or disease earlier so referrals and treatment can be given sooner. In borderline cases, this can hopefully prevent vision loss.
WORTHWHILE INVESTMENT
While insurance reimbursements for many diagnostic tests are being cut, the Diopsys is one test that Medicare and commercial insurers actually reimburse us for, in the range of $180 to $200 for a bilateral VEP or pattern ERG. So the best thing about the Diopsys is that this test is helping me make clinical decisions, and I can actually get paid for helping my patients.
EARLY DIAGNOSIS
Our primary reason for obtaining this technology is to catch diseases earlier. For our patients who are early glaucoma, glaucoma suspect, or who have ocular hypertension, we do visual fields and OCT of the optic nerves. And when there is damage on those, there is already ganglion cell death, and that’s not good for the patient.
So the pattern ERG and VEP pick up damage while the cells are still suffering so I’m able to treat these patient much earlier, when I’m in those borderline states, to hopefully prevent vision loss.
In the end, I’ve been able to use the Diopsys technology for a lot of other conditions, including early age-related macular degeneration or epiretinal membrane, and again in those borderline cases, it helps make the difference.
BETTER OUTCOMES
I’ve actually caught two cases of Plaquenil toxicity—cases I would never have caught—and saved the eyesight of these two patients. Color vision testing, visual field testing, OCT of the macula, they were normal. But with pattern ERG testing, they actually had damage on their low contrast testing and I was able to inform their rheumatologist that they should probably change medications before the cells died resulting in permanent damage.
I also use the Diopsys in early diabetic retinopathy, nonproliferative diabetic retinopathy, where OCT of the macula is normal and they’re seeing fairly well. Since there is no clinically significant macular edema yet, I don’t know if they’re at risk until I refer them to the retinal specialist for treatment. When the pattern ERG shows damage or suggests there might be damage, then I know they need to get that referral earlier.
SOLVES DIFFICULT CASES
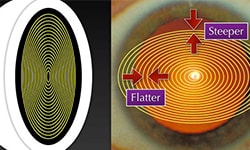
On the pattern ERG, there’s a concentric stimulus and a diffuse contrast setting for different conditions. The focal concentric is more for macular degeneration and drug toxicity like Plaquenil and the diffuse contrast is more for conditions like diabetic retinopathy and any of the glaucomas.
The Visual Evoked Potential module is more for any disease process pre-optic nerve as well as at the optic nerve. So you can also use the VEP in your analysis for glaucoma patients and anything that might be affecting the visual pathway before it hits the optic nerve. In multiple sclerosis patients, I always obtain a baseline VEP so I can decipher if any future optic neuritis event has affected visual function from baseline. It’s also been especially helpful in evaluating patients who are not verbal, or patients who are malingerers, to detect and treat their problems.
If you need to figure out where the problem is, the VEP might decipher if there is something along the visual pathway if everything in the retina and the optic nerve is normal. In other words, it can really help you distinguish in a diagnostic way where visual field testing or OCT of the optic nerve, or OCT of the macula is normal. We’ve found a couple of brain tumors with this technology where the visual field testing was normal. So it’s already impacting a lot of patients in my practice that I would probably have missed without this technology.
MINOR CHALLENGES
While the Diopsys system has wheels that enable it to be moved from room to room within an office when space is needed, it’s not designed to be moved from one office location to another. That’s because the technology could get damaged in a car or truck or other mode of transportation without proper packaging.
Initially, there are some challenges to the set-up of the Diopsys system. As long as you prepare properly, it will connect to your EHR. Just make sure you have a port to plug it into where you intend to put the unit so that your implementation is not delayed. You should also put it a dark, quiet room dedicated to this type of diagnostic testing. But with proper planning, the transition should be very smooth.
Testing with the Diopsys takes at most 10 minutes because the technician has to put a little disposable strip under the patient’s bottom eyelid. The strip doesn’t touch the eye at all, and it’s the only disposable supply you might have to replace down the road. It’s fairly inexpensive once you’ve bought the machine with the only cost is replacing these disposable electrode strips based on usage
FAVORABLE RECOMMENDATION
I would highly recommend the Diopsys system to my colleagues. I wish I knew about it sooner. It’s really electrophysiology as a diagnostic tool, and while it can seem a little overwhelming at first, they’ve made it really simple.
There’s a new module coming out called Flicker ERG that might help determine if taking out the patient’s cataract will help when there is more than one pathology present such as an ERM or early AMD changes. So I can’t wait for that module and I highly recommend this to my colleagues.